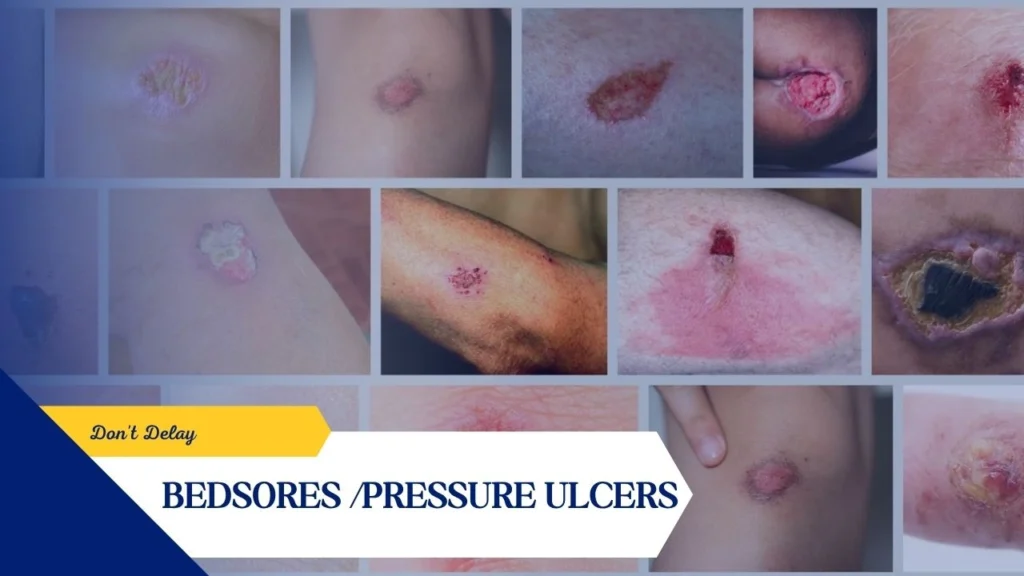
Pressure injuries, also known as bedsores, decubitus ulcers, or pressure ulcers, are localized injuries to the skin and underlying soft tissues that develop due to prolonged pressure, friction, or shear forces. They commonly develop over bony areas such as the hips, sacrum (tailbone), heels, and back.
Management involves relieving pressure on the affected areas, maintaining proper hygiene, and cleaning the wounds with suitable agents such as Calendula or normal saline. The use of appropriate dressings is essential to protect the wound and promote healing. Adequate nutrition plays a vital role; a diet rich in protein, vitamin C, and zinc supports tissue repair and recovery.
Healing time depends on the severity of the ulcer. Stage 1 and 2 ulcers may heal within a few weeks with proper care, whereas Stage 3 and 4 ulcers can take several months and may require advanced interventions such as surgical debridement and infection control.
Bedsores should never be neglected, as delayed treatment can lead to serious complications.
Historically, the condition drew attention from the French physician Jean-Martin Charcot in the 19th century, who observed that patients developing necrotic lesions over the sacrum and buttocks died after some time. He termed this condition “decubitus ominous,” which meant that death was inevitable after developing this lesion.
In 2016, the National Pressure Injury Advisory Panel updated the terminology, replacing “pressure ulcer” with “pressure injury” to better reflect the spectrum of tissue damage, including early-stage injury before visible skin breakdown. This shift highlights the importance of early recognition and intervention.
Etiology & Pathophysiology
The development of pressure injuries is complex and multifactorial, involving both external and internal factors. Externally, prolonged pressure, friction, shear forces, and moisture contribute to tissue deformation and reduced perfusion. Internally, factors such as malnutrition, anemia, dehydration, and endothelial dysfunction accelerate tissue damage. Reduced mobility, excessive skin moisture, poor nutritional status, and impaired sensory perception are among the most significant risk factors. Additionally, advanced age, cognitive impairment, and chronic comorbid conditions further increase susceptibility.
Prolonged pressure exceeding capillary pressure disrupts normal blood circulation, leading to decreased oxygen delivery and accumulation of toxic metabolic byproducts. Over time, this results in tissue ischemia, ulceration, and necrosis. Even as little as two hours of uninterrupted pressure in immobile or bedridden individuals can initiate this process. Impairment of neural mechanisms regulating blood flow also contributes to the progression of these injuries.
Certain patient populations are particularly predisposed, including those with neurological disorders, cardiovascular disease, prolonged immobility due to anesthesia or surgery, dehydration, malnutrition, hypotension, and severe systemic illnesses. In such individuals, tissue tolerance is already compromised, making them highly vulnerable.
At the tissue level, pressure injuries follow a predictable pathophysiological progression. Sustained external pressure exceeding arterial capillary pressure (approximately 32 mm Hg) impedes blood flow, while pressure above venous capillary closing pressure (8–12 mm Hg) obstructs venous return. This dual impairment leads to ischemia and eventual tissue necrosis. The damage often begins in deeper tissues, particularly muscle, before becoming apparent on the skin surface, which can underestimate the severity of the condition during early clinical assessment.
Histologically, these injuries evolve from early erythema (which may be blanchable or non-blanchable) to dermatitis, ulceration, and eventually full-thickness tissue loss with necrosis or gangrene. The earliest changes occur in the microvasculature of the dermis, followed by progressive destruction of skin and underlying structures.
History and Physical
Clinically, patients with intact sensation typically experience discomfort and reposition themselves, thereby preventing injury. However, many affected individuals lack this protective mechanism due to impaired mobility, reduced consciousness, or neurological deficits. As a result, pressure injuries are often first noticed by caregivers. Signs may include discoloration, discharge, foul odor, or staining of clothing and bedding. Notably, muscle tissue may become necrotic before visible skin breakdown occurs, making early detection challenging.
A comprehensive clinical evaluation is essential and should include a detailed history of immobility, duration of hospitalization, underlying medical conditions, and progression of the wound. Conditions such as diabetes mellitus, peripheral vascular disease, and malignancy can significantly delay healing. Assessment should also consider nutritional and hydration status, cognitive function, and mobility.
Evaluation of the wound itself involves careful examination of its size, depth, presence of drainage, necrotic tissue, and any sinus tracts or tunneling. Risk assessment tools play an important role in prevention and management, with the Braden Scale being the most widely used. This scale evaluates sensory perception, mobility, moisture, nutrition, activity level, and friction/shear to determine the patient’s risk category, ranging from mild to very high risk.
Prevention remains the most effective approach in managing pressure injuries. This includes regular repositioning, pressure redistribution using specialized mattresses and cushions, maintaining clean and dry skin, and ensuring adequate nutrition and hydration. Interestingly, studies suggest that repositioning every four hours on advanced support surfaces may be more effective than more frequent repositioning on standard mattresses.
Once a pressure injury develops, treatment focuses on relieving pressure, managing infection, removing necrotic tissue, and promoting optimal wound healing. Offloading the affected area is critical, along with appropriate wound dressings, often silicone-based foam dressings. Debridement is frequently required to remove non-viable tissue and biofilms that hinder healing. However, dry, stable eschar without signs of infection should not be disturbed. While antiseptic agents may be used temporarily, prolonged use can delay healing, and antibiotics are reserved for cases with clear signs of systemic infection.
Nutrition and Wound Healing
Although the exact nutrient requirements for optimal wound healing are not fully defined, increased intake of energy, protein, zinc, and vitamins A, C, and E has been consistently shown to support the healing process. Adequate nutrition plays a crucial role in both the prevention and management of pressure injuries.
High-protein oral nutritional supplements have been found to reduce the incidence of pressure ulcers by approximately 25% in patients at risk. Among all nutrients, protein is the most essential macronutrient, as it is indispensable for tissue repair and regeneration. It is vital for maintaining a positive nitrogen balance and supports all stages of wound healing, including fibroblast proliferation, collagen synthesis, angiogenesis, and immune function.
In enteral nutrition, protein may be provided in the form of intact proteins, hydrolyzed proteins, or free amino acids. Current recommendations by the National Pressure Ulcer Advisory Panel and the European Pressure Ulcer Advisory Panel suggest a daily protein intake of 1.25 to 1.5 g/kg of body weight for general pressure ulcer healing. For patients with Stage III and IV pressure ulcers, the requirement increases to 1.5–2.0 g/kg of body weight per day, depending on the size of the ulcer and the extent of protein loss from draining wounds.
Research has demonstrated that higher protein intake significantly improves healing outcomes. In one study, patients receiving 1.8 g of protein per kilogram of body weight showed nearly twice the rate of wound healing compared to those receiving 1.2 g/kg.
Malnutrition is strongly associated with poor clinical outcomes, increased morbidity, and higher mortality rates in patients with pressure ulcers. It not only delays healing but also increases the risk of complications. Therefore, early identification and prompt management of malnutrition are essential components of effective pressure ulcer care.
The Prognosis of Pressure Injuries
The prognosis of pressure injuries varies widely depending on their stage, location, and the patient’s overall health. Studies indicate that after six months of treatment, approximately 70% of stage 2 injuries heal, compared to about 50% of stage 3 and 30% of stage 4 injuries. Recurrence is common, particularly in sacral ulcers, and long-term preventive care is often necessary.
Complications
Complications are frequent and can be severe, especially in advanced stages. Infection is the most common, with potential progression to deeper structures, resulting in osteomyelitis, septic arthritis, or systemic sepsis. Chronic wounds can also lead to significant protein loss, malnutrition, anemia, and, in rare cases, secondary amyloidosis. These complications significantly increase morbidity and mortality, particularly in elderly patients.
Postoperative and rehabilitative care are equally critical, emphasizing continued pressure relief, proper wound care, nutritional support, and gradual reintroduction of mobility. Successful recovery often requires a multidisciplinary approach involving surgeons, wound care specialists, physicians, physiotherapists, and nursing staff. Family and social support systems also play a vital role in long-term care and prevention.
Here is a serious reminder: pressure injuries are serious, multifactorial conditions that require early recognition, comprehensive management, and sustained preventive efforts. If neglected, they can lead to life-threatening complications, making vigilance and timely intervention absolutely essential. Take care of yourself and your loved ones.
https://www.instagram.com/reel/DXS9fvPknuY/?igsh=MTJkanpzcXhxa3M2cQ==